
Young people are usually less aware of the cancer problem. Many young women get details about breast cancer from stories of others or from TV shows. Very few people decide to study the issue on their own and use professional sources. The majority of the population has little and often too pessimistic visions about prognosis and prevention.
Today mammography is the most informative method for diagnosing breast cancer. Mammoradiologist Danara Muratovna Suleimenova tells about all the ins and outs of this examination.
Danara Muratovna accepts patients as an oncologist-mammologist and as a mammoradiologist. Mammoradiology is a fairly new specialization in our country, a subspecialty of clinical radiology. The mammoradiologist specializes in radiation diagnostics of breast diseases, including ultrasound diagnostics, digital mammography, digital tomosynthesis, MRI, and conducts all types of biopsies. Doctor Suleimenova is receiving patients at the UMIT Oncological Tomotherapy Center, where there is a digital mammography machine with a digital tomosynthesis function.
- Danara Muratovna, what is mammography and what is it used for?
- Mammography is an X-ray examination of mammary glands. Mammography allows to detect early signs of breast cancer (BC). This is the only radiation examination method that has been proven to reduce the likelihood of death from BC. Back in the 60s of the last century in the United States, in the first randomized clinical trial, it was proved that with the help of regular screening mammography, it is possible to reduce mortality from BC by 40%. Since then, many other studies have been carried out in different countries, and all of them have received similar results about the reduction in mortality by 20-40%.
- How is mammography performed?
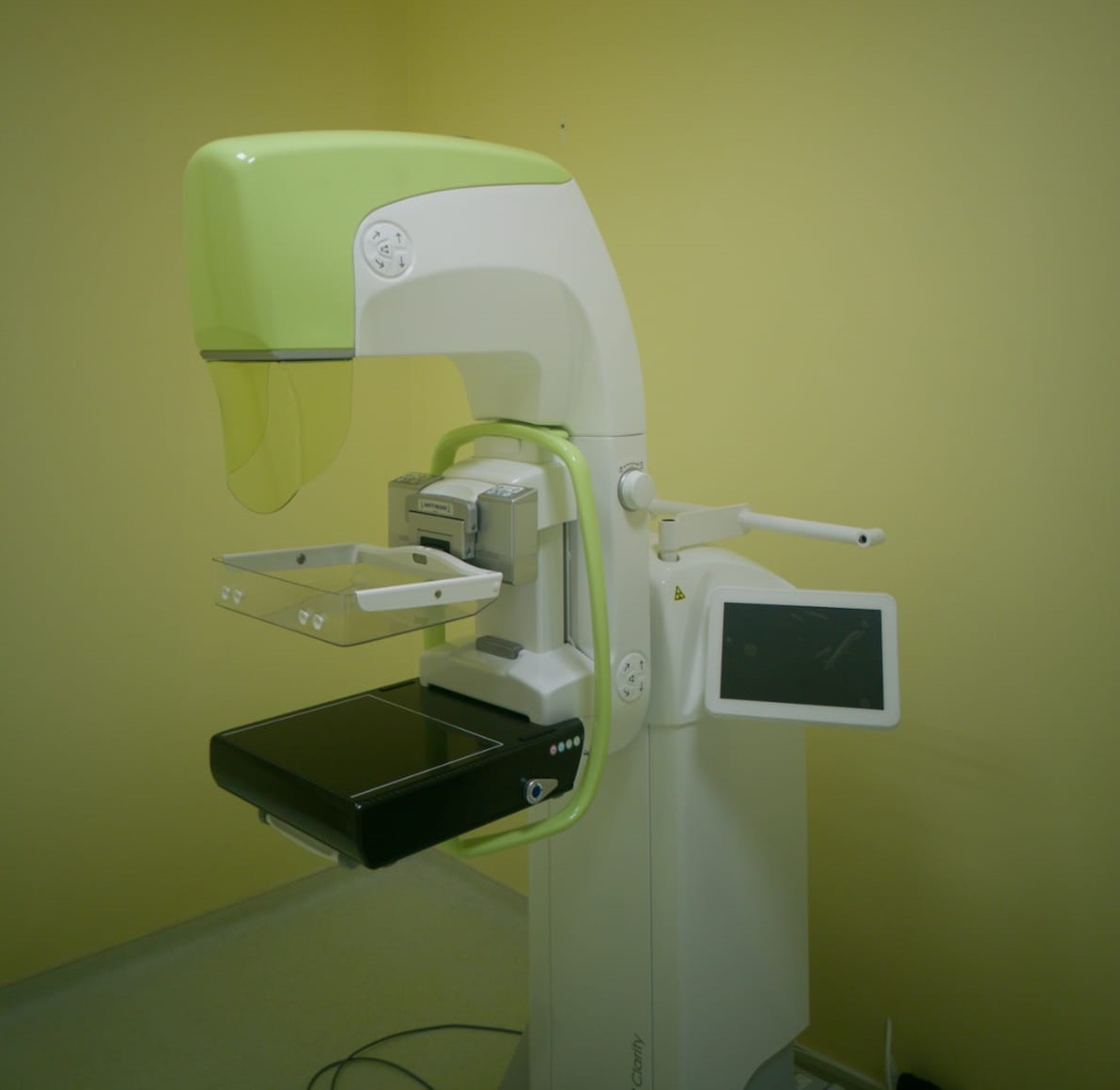
- No special preparation is required for the procedure. Mammography is performed using a special machine - a mammograph. There are analog and digital mammographs. Most modern machines are digital.
Digital mammography has several advantages, such as higher image quality and higher image accuracy. Digital mammographs use lower radiation dose. When a patient undergoes a mammography, she should ask which machine will be used for the examination, and make a choice in favor of digital mammography.
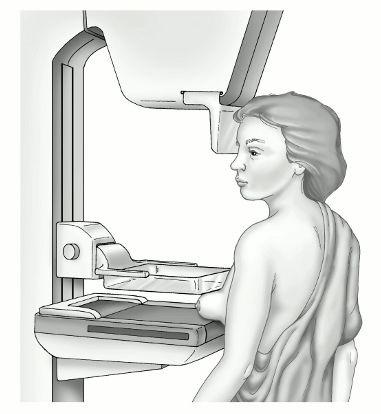
Usually a patient enters the mammography room, undresses to the waist and approaches the machine. The mammary gland is pressed on both sides with special compression plates and an image is taken. The picture itself is taken within a few seconds. The plates are then pulled apart, the breast is released, and the procedure is repeated for the second breast.
In total, two images are taken for each breast, that is, overall, 4 images are obtained. The mammary gland is compressed in two directions: from top to bottom and from the inside to the outside. This is done in order to cover as much tissue as possible, so as not to allow the cancer to go unnoticed, not captured in the field of view.
In addition, one more piece of advice for women: do not use deodorant on the day of the examination, this can create artifacts and on the image it may look like calcifications (accumulation of calcium salts in tissues and organs, as white dots on the images).
- Does it matter on what day of the menstruation cycle do a mammogram?
- No, it doesn't matter at all. Because the information content and effectiveness of mammography do not depend on the day of the cycle. For some reason, it is widely believed in our country that mammography should be done after menstruation. But this is not the case. If there are any formations in the breast, we will see it on any day of the menstruation cycle.
An exception is women whose mammary glands engorge and if there is a severe soreness before menstruation. For such women, in case of a preventive examination, we recommend to come after menstruation in order to reduce pain feelings, when the breast will be more relaxed. But if such women have any complaints, suspicious symptoms, then mammography should not be postponed, it is necessary to undergo it on any day of the cycle.
- What radiation dose does a woman receive during mammography?
- This is a question that often worries women. In modern digital devices, a patient receives the minimum dose of radiation, it is comparable to the dose that a passenger receives during a long flight on an airplane. Such a comparison is given in popular science articles. That is, it is an extremely low dose.
An average dose for standard digital mammography is 0.4–0.5 millisievert, which is much lower than the maximum allowable dose for a diagnostic study. And the doses received by other organs and tissues are extremely low. The safety of mammography for pregnant women has been proven.
Mammography, like any other manipulation in medicine, has potential harm and benefit. There is an X-ray-induced breast cancer, in other words, breast cancer caused by frequent mammography examinations. This is an argument often made by mammography opponents. However, there have been numerous studies that have shown that a woman's risk of dying from a misdiagnosed breast cancer if she does not have a regular mammogram is much higher than the extremely low potential risk of X-ray-induced cancer. The risk-benefit ratio is 1 to 24 according to some data and 1 to 78 according to other sources. That is, the benefits far outweigh the risks.
- After undergoing mammography, conclusions are issued on the BI-RADS scale. What does it mean?
- The BI-RADS scale is a standardized scale for evaluating the results of radiological examination of the breast, which includes ultrasound, mammography and MRI. It was developed by the American College of Radiology (this is a very authoritative organization in the world of radiology) in the 90s of the last century, and since then has proven its convenience and usefulness. BI-RADS is the universal language of mammographers all over the world, it will be understood by a radiologist from any country. This scale is also used in Kazakhstan. A BI-RADS score is required for screening mammography.
I will mention the scale itself, perhaps it will be interesting to readers, because many patients, having received an opinion on BI-RADS in their hands, ask: I have 2/2 - what does it mean? In the BI-RADS scale, there are 7 types of categories from 0 to 6. And with an increase in the category value, the suspicion degree of the detected changes for cancer increases.
BI-RADS 0 – incomplete examination (follow-up examination is required);
BI-RADS 1 – negative;
BI-RADS 2 – benign;
BI-RADS 3 – probably benign, but follow-up is required;
BI-RADS 4 and 5 – suspicion of cancer, biopsy is required;
BI-RADS 6 – proven malignancy, after biopsy.
The conclusion may sound something like this: "Nodule formation of the right mammary gland BI-RADS 4". And further, recommendations related to this category must be indicated. In the BI-RADS system, if the doctor has assigned category 4 or 5, he is obliged to recommend a biopsy.
- Is it possible to have mammography for women with breast implants?
- This is also one of the most widespread myths in mammology - that women with implants cannot undergo mammography. There are absolutely no differences in the recommendations for examination, including for undergoing mammography, for women with and without implants. Mammography is the only method that can detect early tumors such as in situ, or "in situ cancer" that manifests itself as microcalcifications. These microcalcifications are not visible either on ultrasound or even on MRI. Therefore, mammography is indicated for all women, including women with implants.
But there are differences: women with implants are recommended to be examined on digital devices with a special function "implants". Why is it important? Because the "implants" function allows to optimize the compression, i.e. compression of the mammary glands to reduce the risk of damage to the implants. In modern mammology, there are practically no cases of damage to implants.
Another difference is that 4 additional projections are taken for the breast with implants. For the first time, all 4 pictures are taken as usual, i.e. both the breast and the implant in it. And then a specially trained X-ray laboratory assistant pushes the implant back, and the breast tissue itself is pulled forward, and 4 more pictures of the breast itself are taken without the implant.
- When is mammography contraindicated?
- In fact, there are no absolute contraindications - neither pregnancy nor breastfeeding interferes with the examination. But nevertheless, according to the recommendations, screening, as a preventive examination, is not done during pregnancy. But if a pregnant woman has a lump in the breast, then such a patient is first examined for an ultrasound scan, and if there is a suspicious formation, she is sent for mammography.
Lactation is also not a contraindication for mammography. There will be no harm to either the breastfeeding woman or the baby. One difference - it is recommended to express milk or feed the baby before mammography, to prevent reducing the information content of the images.
- Can radiation dose after mammography remain in milk?
- Absolutely not. Stopping breastfeeding during the examination is not required at all.
- What are the rules for screening in Kazakhstan?
- According to the Kazakhstan National Screening Program, women from 40 to 70 years old are examined once every two years. They should be called by the polyclinics to which they are attached. After the age of 70, the screening program does not work, but we recommend that women over 70 undergo a mammogram themselves. If you go to your clinic and ask for a mammogram, no one will refuse you.
- Why is it necessary to start regularly undergoing mammography at the age of 40, and not earlier?
- A woman's mammary gland consists of three types of tissue: fat, the glandular tissue itself, and the connective tissue that supports the mammary gland. And the ratio of these three types of tissue at different ages is different. In young women, glandular tissue predominates and it is the glandular tissue that is most sensitive to the effects of ionizing radiation. A young woman will have more potential harm from a mammogram than an older woman. This is the first argument why mammograms are only started after 40 years. And the second - the glandular tissue looks white on mammography. Similarly, cancer, fibroadenoma, cyst look white. Of course, when white is on white, it makes it difficult to diagnose.
With age, the glandular tissue of the mammary gland is replaced by the fatty tissue, as the process of age-related involution takes place. Fatty tissue on mammography looks black, and on a black background, any neoplasm, even a tiny one, will be clearly visible.

- Let's summarize, what are the pros and cons of mammography? After all, there are problems of false-negative and false-positive results, over-diagnosis and over-treatment.
- The advantages of mammography are obvious: it is an early diagnosis of cancer and, accordingly, less aggressive treatment and a better prognosis. This is good for both women and society: we prevent disability, women can remain socially active, and the state preserves budget funds.
Among the minuses, we can name the irradiation, as well as false-negative and false-positive results.
What are the false-positive results? For example, a woman underwent the screening, we saw some kind of suspicious, in our opinion, formation. The patient was invited for an additional examination (ultrasound and targeted mammography), and afterwards they were convinced that it was a cyst or just an overlay of shadows. This false-positive result is not dangerous in itself, but causes anxiety and stress in the woman until she receives a final conclusion that everything is fine with her.
With regard to over-diagnosis and over-treatment. There cancer "in situ" (pre-invasive cancer, intraepithelial cancer or stage 0 cancer - a malignant tumor at the initial stages, a feature of which is the accumulation of histologically altered cells without invading the underlying tissue). There is some disagreement among scientists about whether cancer in situ can be considered cancer, whether cancer in situ can develop into an invasive form, metastasize, or whether aggressive anti-cancer treatment is worth starting. But we can't say for sure. In modern medicine, there are no tools with which it is possible to determine which cancer in situ will develop into invasive, and which will not grow and remain in place, and will not progress for many years. And therefore, since we do not have such differential markers, we treat all breast cancers according to the standard. That is, if we find cancer in situ, then we treat it.
Now an interesting study is being carried out in the world - women with cancer in situ were divided into two groups. One group is treated according to the standard, and the second group is simply monitored. And now all of us, doctors, are waiting for the results of these studies. In total, there are five such studies in the world at the moment. We do not yet know what the results will be. But I can say that researchers have a big problem with recruiting patients. Because few people with cancer in situ want to go to a group that is simply being watched and not treated. Still, in women, cancer in situ is associated with danger.
I had a patient, an American woman, diagnosed with cancer in situ in 2017, she had calcifications on mammography. She had her own approach to health, she practiced meditation. And although all the doctors recommended her surgery, she refused treatment. For work, she was sent to Kazakhstan and was recently examined by me. I saw that the calcifications increased in quantity and size. We performed the second biopsy, and, unfortunately, we have already diagnosed invasive cancer.
So far, the traditional approach in medicine says that cancer in situ should be treated according to the classical canons of oncology.
- The woman underwent mammography. What do the images show? What exactly is the doctor looking for on a mammogram?
- On the images, first of all, we evaluate the two mammary glands for symmetry, because some types of cancer can manifest themselves only in the form of tissues asymmetry. In addition, we are looking for nodular lesions, they appear in the form of shadows. A shadow is a lighter area against the dark surrounding tissue. A distinct boundary of the shadow is characteristic for benign formations, fibroadenomas, an indistinct boundary is more suspicious of cancer.
In addition to nodular masses, we are also looking for calcifications. The majority of women have their established opinion that calcifications on a mammogram are something dangerous associated with cancer. It must be understood that most of the calcifications are benign. They are associated with calcification of the vascular walls, with dystrophic processes in the mammary gland, with fibrocystic mastopathy and are not a sign of cancer. Only a trained radiologist can recognize which calcifications a woman has. Cancer calcifications may be said, the waste products of cancer. A cancer cell dies during its life, and due to metabolic processes, calcium begins to be deposited around it.
But I must say that not all tumors give calcifications. Cancer can also manifest itself as a violation of the architectonics, tissue structure.
- Suppose, a certain formation is found on mammography, what is next?
- First of all, an ultrasound examination is carried out for a woman, aimed at suspicious areas. An ultrasound scan either confirms that a suspicious lesion actually requires a biopsy, or that there is nothing dangerous.
- When is the biopsy performed?
- There are two types of biopsies. Fine-needle - aspiration biopsy, and core-needle, or trepanobiopsy. When we talk about a puncture, this is a fine-needle biopsy. Previously, such a puncture was used to diagnose cancer because there was no alternative. Trepanobiopsy has now replaced it. And the gold standard for cancer diagnostics is trepanobiopsy. Dear women, pay attention to this: if you have a formation in your breast and the doctor offers to have a puncture, you can refuse, because the puncture is not informative.
During trepanobiopsy, we take pieces of tissue and from them we can tell with an accuracy of 99.9% what kind of tissue it is. And during puncture, we only take cells. It is very difficult to make a diagnosis based on such data.
- Tell us about tomosynthesis
- Tomosynthesis has been introduced in Kazakhstan relatively recently, since 2017. Now there are about 10 digital mammography machines with tomosynthesis function in the country. I would like to immediately put all the dots on the "i". Tomosynthesis is not an examination method, it is a screening method. It is much more informative than conventional mammography, detects one and a half to two times more cases of cancer than mammography. And it gives fewer false-positive results. Tomosynthesis is good precisely as a primary diagnostic method. For preventive examination, definitely choose tomosynthesis.
- Due to what features the tomosynthesis is more informative than mammography?
- With conventional mammography, we compress the breast on the top and on the bottom and shoot in one projection. And with tomosynthesis, the machine moves in an arc and produces a number of images, from 9 to 15, depending on the manufacturer. After that, a special algorithm reconstructs these images into pseudo-3D images of breast tissue.
Tomosynthesis has more gentle compression. In general, compression in mammography has two purposes. The first is to get a distinct image: the more the compression, the clearer is the image. The second purpose of compression is to reduce the radiation dose absorbed by the breast. The higher the pressure, the lower the dose. During tomosynthesis, in order to get a distinct image, it is not necessary to apply strong compression. In fact, compression is only used for fixation.
The more frequent detection of tumors is also due to the fact that we get slices only 1 mm thick - the likelihood of missing white cancer against the background of a white breast is much less.
During tomosynthesis, over-diagnosis is minimized - tomosynthesis detects more invasive cancers than conventional mammography and reduces the likelihood of errors. And at the same time, the radiation dose is similar to that of a conventional mammography.
Tomosynthesis allows to detect smaller formations than standard mammography, so we are talking about an earlier detection of breast cancer.
- How to get to tomosynthesis?
- At the UMIT Oncological Tomotherapy Center (Nur-Sultan) there is a digital mammography machine with a tomosynthesis function manufactured by Planmed (Finland). You can contact our center and undergo this highly sensitive and safe breast examination method.
You may be interested in articles on this topic:
UMIT Oncological Tomotherapy Center passed JCI International Accreditation