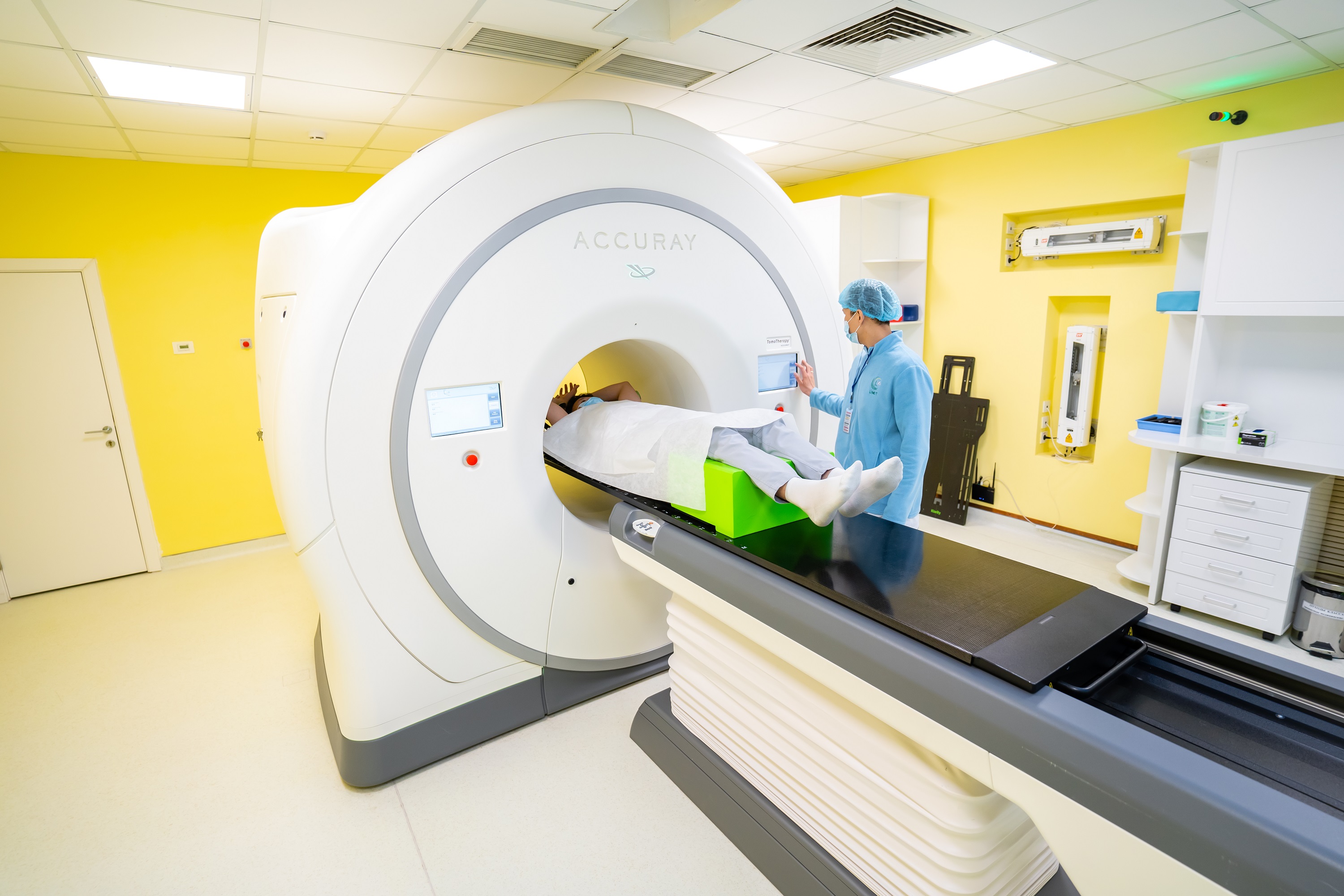
 The UMIT Oncological Tomotherapy Center is modeled on the best European clinics. The innovative TomoTherapy HD radiation therapy machines manufactured by Accuray (USA) are installed here. Tomotherapy has raised the understanding of the cancer patients comfort and their quality of life to a completely new level.
The UMIT Oncological Tomotherapy Center is modeled on the best European clinics. The innovative TomoTherapy HD radiation therapy machines manufactured by Accuray (USA) are installed here. Tomotherapy has raised the understanding of the cancer patients comfort and their quality of life to a completely new level.
What is tomotherapy and how it works, explained the director of the UMIT Oncological Tomotherapy Center, Yerzhan Mukatayevich Shayakhmetov.

– Tomotherapy is called one of the revolutionary solutions in the history of radiation therapy. What is this statement based on?
– Today, tomotherapy is the gold standard for the radiological treatment of cancer patients. This is a modern device for radiation therapy of carcinomas, which combines a linear accelerator and a computed tomograph. Technically, this is a completely new approach due to three key points:
The first one is a unique system of irradiation with a fan beam of high energy photons in a spiral order.
The second is a narrow, intensity-modulated irradiation field.
The third is the simultaneous rotation of the radiation source and the movement of the table with the patient.
The equipment used for TomoTherapy HD looks very much like a computed tomography (CT) system. During treatment, the patient lies on a couch that moves continuously through a rotating ring. Radiation spreads from all directions as the ring rotates and the couch moves through the portal.
– Yerzhan Mukatayevich, let's consider each of the tomotherapy advantages and try to understand what they are better at.
Tomotherapy has fewer side effects compared to other linear accelerators
– Reducing side effects is achieved due to the fact that the tomotherapy machine has a narrower radiation field with modulated intensity and additional improved visualization. This feature allows to maximize the protection of healthy tissues surrounding the tumor.
During tomotherapy the maximum therapeutic dose hits the tumor exactly
– This is achieved through a unique spiral irradiation method and a multi-leaf collimator. Irradiation begins from the edges of the tumor and, rotating in a spiral, gradually reaches the center of the tumor. Irradiation goes spirally from different planes. Due to this, absolutely the entire tumor is equally irradiated from all sides. For one fraction, the irradiating dose of photons is not scattered anywhere and hits the tumor exactly. On conventional linear accelerators, the irradiation is pyramidal, only from one plane.
The innovative Multi-Leaf Collimator (MLC) consists of many leaves, we call them "shutters". Every 20 milliseconds, these shutters open, let the beam pass, and close. That is, the beam does not hit constantly, it goes alternately, every 20 milliseconds the required dose hits exactly where it should go. The dose is distributed evenly, and, importantly, the maximum radiation dose reaches the tumor. Not a part of the tumor is left untreated.
Tomotherapy allows to irradiate tumors of very complex forms and large sizes during one session
– This accuracy depends on the work of the whole team. Radiologists carry out careful planning, computer simulation is carried out, the contours of the tumor and its borders are determined, because tumors can be of different sizes and different shapes, can affect neighboring organs and tissues. Thus, radiation oncologists outline the tumor on a computer using a special program, creating a 3D model of the tumor. Medical physicists then plan to deliver the dose to the tumor. This work is very important. When a patient undergoes irradiation, the entire contoured tumor is irradiated, no matter how complex and large it is, without leaving its boundaries.
Tomotherapy allows a simultaneous irradiation of multiple metastases
– Computed tomograph allows to create three-dimensional models of each metastasis and identify their localization in the body. Therefore, using the tomotherapy machine, it is possible to simultaneously treat metastases in different parts of the body, while maintaining high accuracy of irradiation and delivery of the required therapeutic dose to each metastasis.
Visual control of treatment during tomotherapy
– Three-dimensional CT scans give us visualization - we know exactly the size and location of the tumor, and therefore during tomotherapy we can track any changes, that is, we can determine the tumor's response to radiation. And if necessary, we can easily and quickly change the treatment plan.
Tomotherapy is the only radiation method for patients with pacemakers
– Very often, cardiac patients are given pacemakers, or artificial defibrillators so that the heart works smoothly in an automatic mode. But in case of tumors in the mediastinum, esophagus or lungs, irradiation of patients with pacemakers cannot be carried out on conventional linear installations, since the batteries on these devices may fail. The tomotherapy machine allows to reach the tumor without touching the pacemakers, bypassing them. According to the rules, pacemakers should not be allowed to be exposed to more than two or three grays. So, our physicists have achieved an impressive result: the total dose that falls on artificial pacemakers and defibrillators reaches only 0.5 gray.

– What is the preparation for treatment consists of?
– During tomotherapy, it is very important to keep the patient still in order to achieve maximum results. If, for example, a patient comes for treatment during 20 days, on each of these days he should take the same position during the tomotherapy and not to move. To achieve this, an individual fixation device is made for each patient - a thermoplastic mask and a vacuum mattress. Mattresses and masks help to maintain immobility of a patient, repeat all the bends of the body, fix the position.
The second important point. After the calculations of physicists and radiologists, irradiation is not performed immediately on the patient. We have a phantom, a special device that is able to read all the data and give a conclusion that the calculations have been carried out correctly and it is possible to start treating a patient.
This increases the treatment safety and provides less radiation exposure to patients.
– What type of radiation is used in tomotherapy machines and how does it affect cancer cells?
– In today’s radiation treatment on linear accelerators and tomo machines, the energy of photons is used. During irradiation of cancer cells, the DNA chain is destroyed, and subsequently the tumor cell stops multiplying and growing. Thus, the destruction of the tumor occurs.
– How many tomotherapy sessions may a patient need?
– We call them fractions. For different types of oncological diseases, a different number of fractions is carried out, the number can reach up to 40 fractions.
In the palliative mode, from three to 20 fractions are performed. That is, in advanced stages, when it is already impossible to irradiate strongly, when there are multiple metastases, the tomotherapy helps to relieve pain syndrome, to alleviate the patient's condition.
– What types of cancer can be treated with tomotherapy?
– In fact, we can treat almost all types of cancer, almost all localizations, except for ovarian cancer, since there is a different nature of the disease that requires surgery and chemotherapy.
We treat tumors of the brain, spinal cord, breast cancer, esophageal cancer, lung cancer, pleural mesothelioma - in this case, tomotherapy is considered the gold standard of treatment.
Also, tomotherapy is the only method of total bone marrow irradiation for leukemia in children and adults. Before the transplantation of bone marrow, total radiation is performed, and this allows to achieve much better results in the treatment of leukemia. We can treat children from one and a half years old.
In addition, there is a group of palliative cancer patients, whose metastases cause discomfort, pain, and significantly worsen the quality of life. Then, using a tomotherapy machine, we can point-irradiate a metastasis, for example, an affected vertebra, and this greatly relieves pain. We do not actually treat the tumor, but we make the patient's condition easier, thereby improving his quality of life. This is a palliative treatment regimen.
– What patients are not allowed for tomotherapy treatment?
– We refuse tomotherapy to patients at the fourth stage, with multiple organ lesions, with multiple metastases, with cancer intoxication, with cancer cachexia - radiation is already contraindicated for such patients.
– Are there any side effects of tomotherapy?
–Mainly they are local skin manifestations: dermatitis, epidermitis, they disappear over time. For example, after irradiation of the rectum, post-radiation rectitis or proctitis may develop.
But I can say that during two years, while treating cervical cancer, we have never received complications that can occur with irradiation on other devices (so-called fistulas - recto-vaginal or recto-urinary fistulas, cervico-rectal fistulas).

– How to get a quota for treatment at UMIT Oncological Tomotherapy Center?
- Firstly, it is necessary to be registered at the oncology dispensary at the place of residence. Secondly, it is necessary to have a multidisciplinary team's decision to perfrom the radiation therapy. Thirdly, the patient's desire to come to Astana and undergo treatment in our tomotherapy center is needed.
Usually, radiologists at the patient's place of residence contact us and give copies of all documents. You can write to our e-mail: info@tomo.kz. Our radiologists consider, analyze it, ask for additional tests, if necessary, and then, in case of a positive decision on the allocation of a quota, they report that the patient can come for treatment.
In our UMIT Oncological Tomotherapy Center there is a certain annual number of quotas for the state order. For each patient, the final decision on the allocation of quotas is made by our center. If the annual number of quotas ends in a shorter time, then we can make a request from the state for an additional amount of quotas. For two years so far the state has not refused us. For our part, we fully comply with all contractual obligations to the state.
– If a patient applies on a paid basis, how much will the treatment cost?
– I must say firstly, that a consultation of a radiologist is free. We can offer paid tomotherapy services to oncology patients with the fourth stage or those registered in the dispensary, as the fourth clinical group. These are usually extremely difficult patients, they are not indicated for quota treatment. For such a group of patients, provided that their condition allows, we can help with severe pain syndrome, for example, conduct two or three fractions of radiation in order to alleviate the condition. These patients have to pay themselves.
One fraction consists of approximately 250-260 thousand tenge. This amount includes the whole range of services, including all analyzes, examination, production of a fixing mattress and a mask.
– Do you accept citizens of other countries for treatment?
– Yes, we do, on a paid basis. We had patients from Uzbekistan, Kyrgyzstan. Citizens of neighboring countries can write to our e-mail and send their documents. The rest of the registration process is the same as for our citizens. In Central Asia, our center is the first and only center for tomotherapy.
By the way, I must say that in 2020 we passed national accreditation and received the highest category in Kazakhstan. We are now preparing for the international accreditation according to JCI standards for patient and physician safety. This will give us the opportunity to be included in the international register of medical centers accredited for patient safety standards. We will be able to freely accept foreign patients.
– How many patients can a tomo machine treat in a year?
– Our tomotherapy machine can be used to treat up to 100 people a day.
In 2019, we treated 205 people. Of these, 61% underwent radical therapy (until the tumor was completely destroyed), 38% underwent palliative care (severe patients at the last stages).
In 2020, 444 patients were treated, which is twice as many. 70% of them went through a radical scheme. That is, there was an understanding that the earlier treatment is started, the better the results. Due to the wide notification of the regions, doctors began to send patients to us at earlier stages.
It should be noted that today among newly diagnosed cancer patients 70% require radiation therapy. This is a very large figure. In 2018, 182 thousand people were registered, of which the first identified are almost 34 thousand people. So, 70% of these 34 thousand patients need radiation therapy.
– Yerzhan Mukatayevich, what do you, as an oncologist, recommend to people as a preventive measure?
I want to say to people: you need to love yourself, take care of your health, and when a certain age comes, for example, from 35 years old you need to undergo all screening tests. There are three of them now, all available and free - for breast cancer, cervical cancer and prostate cancer, they must be undergone.
As an oncologist, I will say that breast screening really works, do not underestimate it. In 2009, breast cancer in the first or second stage was 20-25%. And the third-fourth stage accounted for almost 70%. After the introduction of breast cancer screening throughout Kazakhstan, by 2015 there were already figures that the first-second stage of breast cancer was 70%, and the third-fourth stage was 30%. On a national scale, these are very important changes.
– Many people are very worried about the question: can a person become radioactive during treatment? Sometimes relatives try to avoid close contact with people receiving radiation therapy.
– At our center, we have specially issued a brochure for patients, which explains in detail what radiation therapy is, how to behave, how to eat, how to live with it. Our patients undergo only outpatient treatment. They come to us at the appointed time, undergo an examination, take a treatment fraction and go home.
I want to say that radiation therapy a priori does not bring any burden or threat to other people. This is the energy of photons, this is the energy of the sun. We do not use any radioactive means, isotopes, so there is no radiation. It poses no threat to others. Photons pass through the body, do not linger anywhere, do not accumulate.
– Your center is called "UMIT" – that means hope.
– "UMIT" - because our center wants to give people the hope that there is a chance to get modern effective treatment and recover from the disease, and this is our mission - "Add a new hope on the way toward healing with us!" And the snowdrop on the clinic's logo is a symbol of faith that, despite the snow and cold, spring, sun and warmth will come!
You may be interested in articles on this topic:
UMIT Oncological Tomotherapy Center passed JCI International Accreditation